Noisy Knees: What Does Knee Crepitus Mean for Your Joint Health?
Do your knees make snapping, crackling, or grinding noises when you move? If so, you’re not alone. A recent systematic review and meta-analysis revealed that knee crepitus (the audible or palpable sounds from the knee joint) is surprisingly common, affecting up to 41% of the general population and 81% of people with knee osteoarthritis (OA). But is that noise something to worry about? Let’s explore what knee crepitus means, its link to structural pathology, and how we can help you keep your knees healthy and pain-free.
What Is Knee Crepitus?
Knee crepitus refers to the sounds (pops, clicks, or grinding) or sensations that occur when the knee moves. While it can happen at any age and to anyone, the review highlights that it’s particularly prevalent in:
• Pain-free individuals: 36%
• People with ligament injuries: 35%
• Those with cartilage pathology: 61%
• Individuals with knee osteoarthritis: 81%
These noises often raise concerns about underlying joint damage, especially when they’re accompanied by pain, stiffness, or reduced mobility.
What Causes Knee Crepitus?
Knee crepitus can have several causes, some benign and others linked to structural issues in the joint. Common causes include:
1. Benign Crepitus: Often due to gas bubbles popping in the joint or normal movement of tendons and ligaments over bony structures.
2. Cartilage Changes: In conditions like osteoarthritis, cartilage may break down, leading to irregular joint surfaces that produce grinding noises.
3. Joint Effusion or Swelling: Excess fluid in the knee can alter movement mechanics.
4. Ligament Injuries or Weakness: These can lead to instability and abnormal joint movement.
5. Muscle Imbalances: Imbalanced strength or tightness in surrounding muscles can impact knee mechanics.
Is Noisy Knees a Sign of Trouble?
While knee crepitus is not always a cause for concern, the study found that individuals with noisy knees have a 3.79 times higher likelihood of having radiographic osteoarthritis and may exhibit features of OA on MRI. This means that knee crepitus could be an early indicator of joint changes, making it important to address before symptoms progress.
What Can Be Done About Knee Crepitus?
If knee noises are causing discomfort or concern, early intervention is key to maintaining long-term joint health. At The Body Lab, we take a comprehensive approach to assessing and treating knee issues. Here’s how we can help:
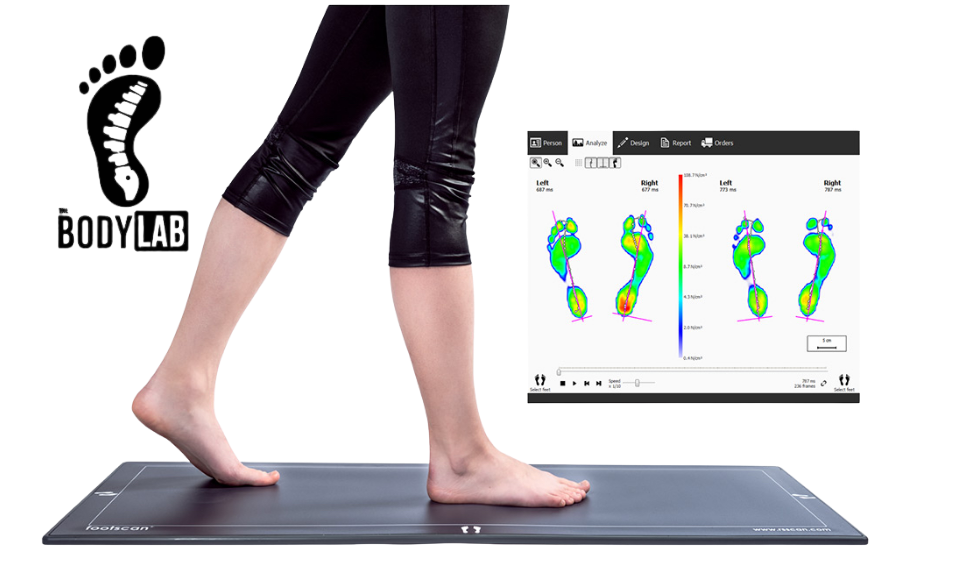
1. Movement Assessments: We analyze your gait and knee mechanics to identify imbalances or compensations contributing to crepitus.
2. Targeted Treatments:
• Acupuncture: To reduce inflammation and improve blood flow to the joint.
• Movement Therapy: Corrective exercises to optimize joint alignment and muscle activation.
• Biomechanics Education: Helping you understand how to move efficiently and protect your knees.
3. Strengthening & Stability Work: Building muscle strength around the knee to reduce strain on the joint and improve stability.
4. Foot & Hip Mechanics: Since the knee connects the hip and foot, we assess how these areas contribute to your knee health.
Why Choose The Body Lab?
At The Body Lab, we focus on root-cause solutions rather than short-term fixes. Whether your knee crepitus is caused by early joint degeneration, muscle imbalances, or poor movement patterns, we’ll create a tailored plan to help you regain pain-free motion and long-term joint health.
Book Your Knee Health Assessment Today!
If you’re worried about noisy knees or want to improve your joint health, schedule an assessment with us. Let’s address the root of the issue before it leads to more serious problems. Your knees will thank you!
REFERRENCE : https://bjsm.bmj.com/content/59/2/126.abstractThink posture is about sitting up straight? Think again. Posture isn’t a position—it’s a reflection of what your body can feel, move, and control. In this article, we break down what posture really is, why your nervous system is calling the shots, and how movement—not stiffness—is the key to changing it.
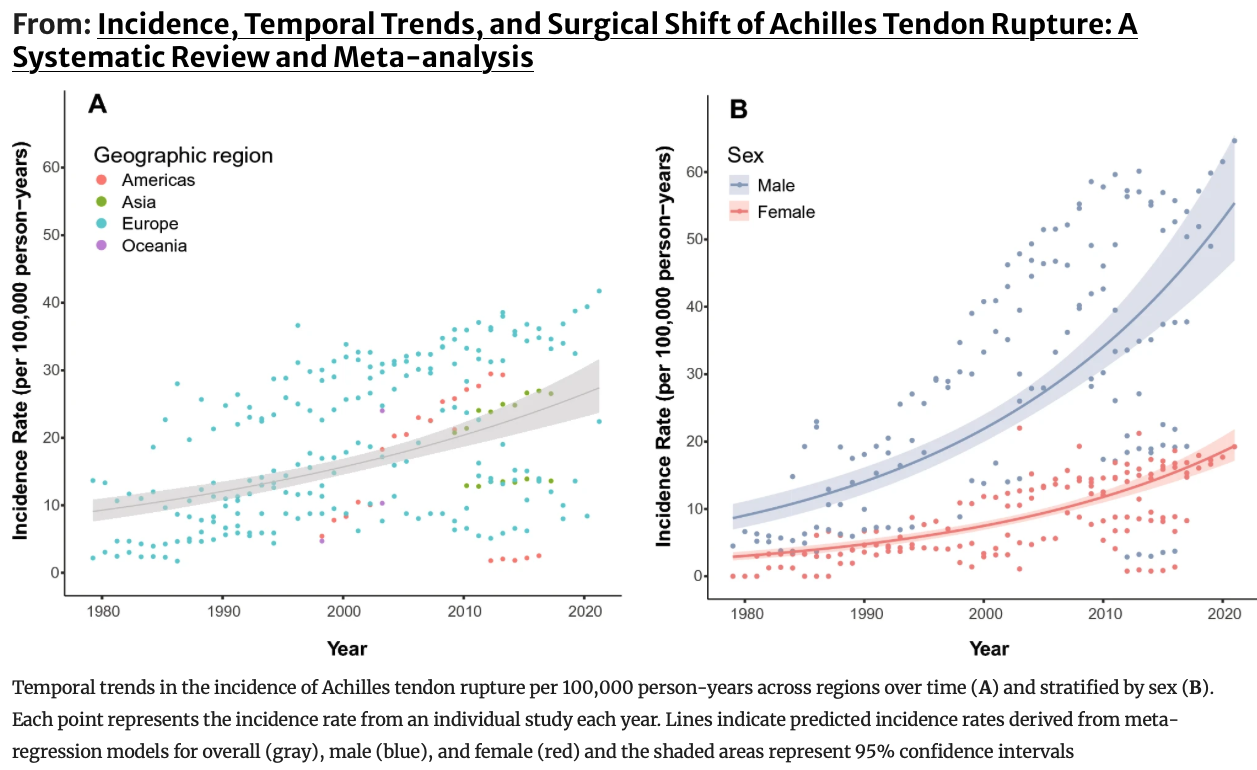
Achilles tendon ruptures are increasing worldwide. Learn why it’s happening, what the latest research shows, and how to improve tendon strength, foot mechanics, and prevent injury.
Struggling with bone loss or worried about osteoporosis? Learn how strength training, impact exercise, and balance work can improve bone health. Insights from Canberra physios at Next Gen.
Discover how foot pressure plate analysis in Canberra reveals how you walk, move, and load your body. Advanced gait assessment at The Body Lab.
A 2025 study suggests stimulating lymphatic vessels in the neck can double brain waste clearance—but before you start massaging your face non-stop, let’s break down what the research actually shows. From sleep and movement to fluid dynamics, this guide explains how your body really supports brain health—and where therapy fits in.
Cluster headaches are severe, recurring, and often resistant to medication. This guide explores how acupuncture and cranial therapy in Canberra can help reduce pain, frequency, and improve long-term outcomes.
Poor sleep affects hormones, metabolism, pain, and recovery. Evidence-based insights with Australian sleep data and metabolic perspective.
Persistent pain is not always caused by tight muscles or stiff joints. In many cases the nervous system and skin play a key role. Understanding this connection can change how chronic pain is treated.
Dermo-Neuro Modulating is a gentle manual therapy technique that works through the skin to calm irritated nerves and reduce pain. Developed by physiotherapist Diane Jacobs, it offers a modern, neuroscience-informed approach to treating persistent pain conditions.
Ankle sprains are often treated as ligament injuries, but the mechanics of the foot tell a much bigger story. One structure that frequently goes unnoticed is the Flexor Hallucis Longus (FHL) — the tendon that connects the calf to the big toe and plays a critical role in propulsion, arch stability, and walking efficiency. Because this tendon runs through a narrow tunnel behind the ankle joint, it can be compressed or irritated during common inversion ankle sprains. Understanding how the FHL contributes to foot mechanics may help explain persistent ankle stiffness, reduced push-off power, and ongoing pain after injury. Exploring the role of the big toe in ankle recovery offers a more complete view of foot biomechanics and movement rehabilitation.
If you’ve ever searched “acupuncture for pain Canberra”, chances are something in your body has decided it’s had enough. Maybe it’s your heel barking every morning, a shoulder that refuses to behave, or a lower back that stiffens the moment you sit down too long.
Acupuncture can be remarkably effective for reducing pain. But here’s the honest truth most clinics won’t say out loud:
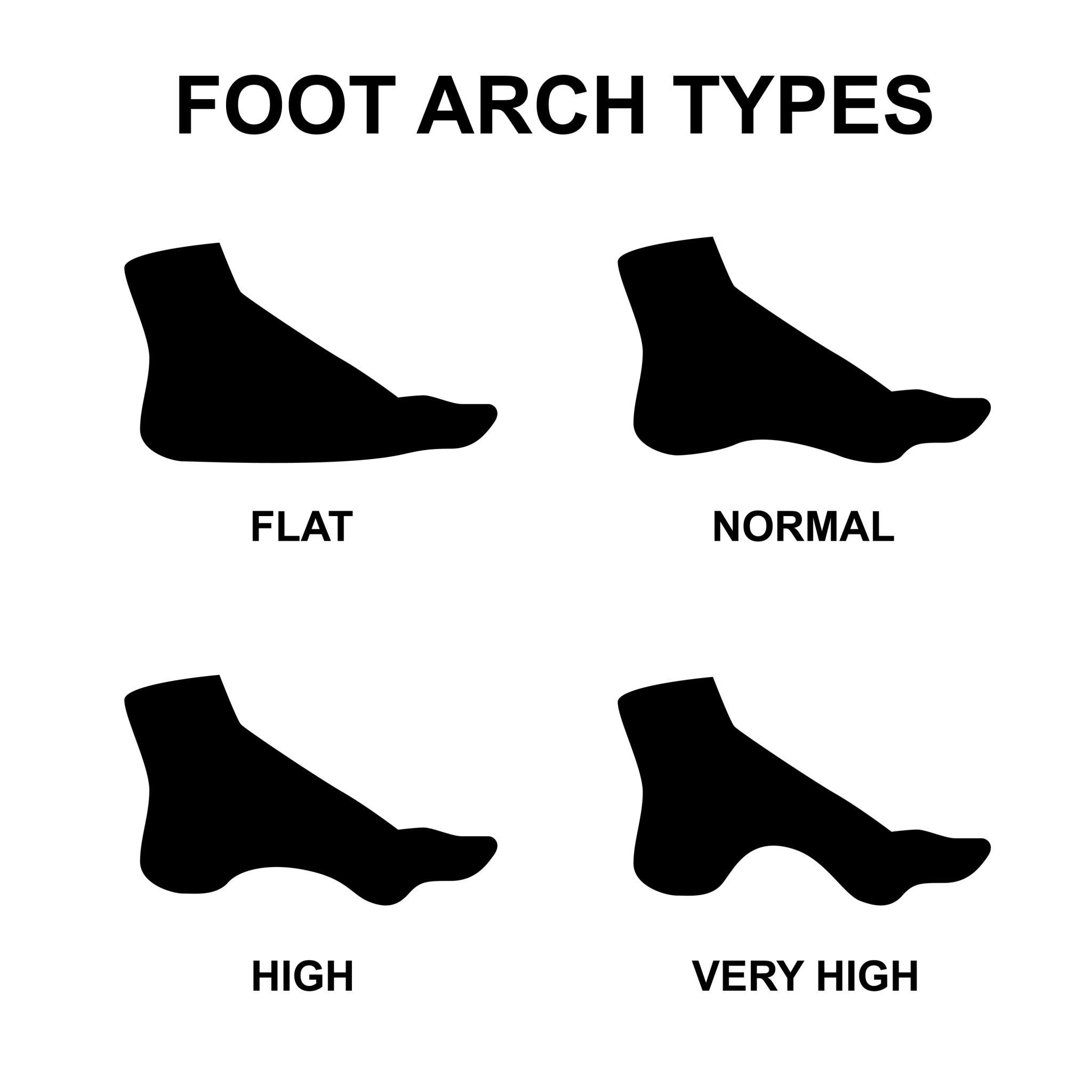
Foot shape plays an important role in how the foot absorbs force and distributes pressure during walking. From flatter pes planus feet to the higher-arched pes cavus foot type, these structural differences influence how load travels through the heel and arch.
Understanding how these loading patterns affect the tissues around the heel—including the plantar fascia and Baxter’s nerve—may help explain why some people develop persistent heel pain while others do not.
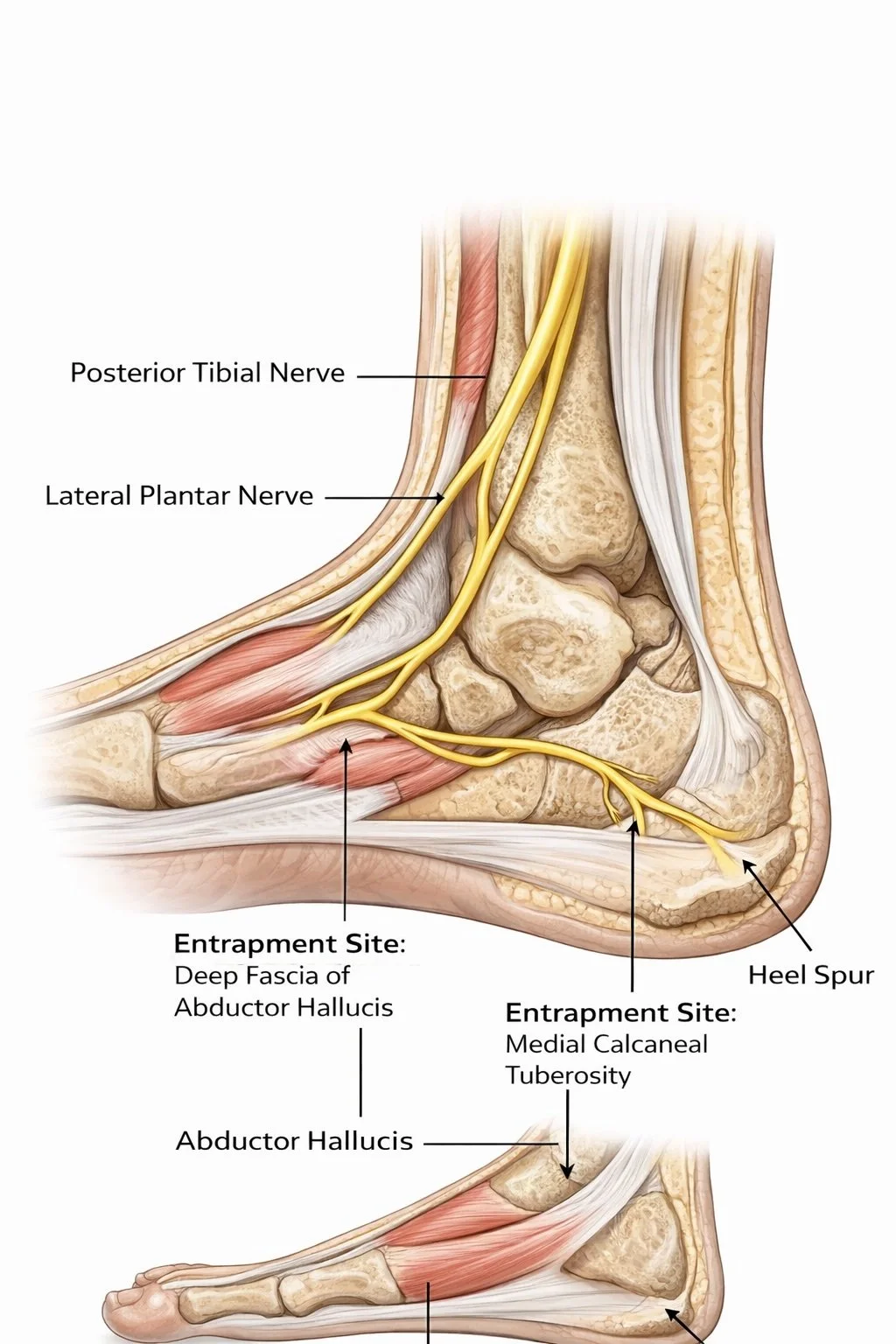
Most cases of heel pain are quickly labelled plantar fasciitis, but that diagnosis doesn’t always tell the full story.
Research suggests that Baxter’s nerve entrapment—compression of the inferior calcaneal nerve—may account for up to 20% of chronic heel pain cases. Because the symptoms overlap with plantar fasciitis, this nerve condition is frequently overlooked.
Understanding how gait mechanics and medial heel loading influence the tissues surrounding Baxter’s nerve can help explain why some heel pain persists despite traditional treatments.
Most cases of heel pain are quickly labelled plantar fasciitis, but that diagnosis doesn’t always tell the full story.In fact, research suggests that up to 20% of chronic heel pain cases may involve compression of Baxter’s nerve, a small branch of the lateral plantar nerve that runs along the inside of the heel. Because the symptoms overlap, Baxter’s nerve entrapment is frequently mistaken for plantar fasciitis.While plantar fasciitis involves irritation of the plantar fascia, Baxter’s neuropathy is a nerve compression problem, which means the symptoms, mechanics and treatment considerations can be quite different.
Understanding the difference is important. Treatments designed for plantar fascia inflammation may not help nerve-related heel pain—and in some cases may even aggravate the underlying problem.
In this article we explore the key anatomical and biomechanical differences between these two conditions and explain why a deeper look at foot mechanics and gait can be crucial when heel pain persists.
Heel pain when walking is one of the most common problems I see at The Body Lab in Canberra. Here’s why it happens and how improving foot mechanics can help.
Foot pain is often treated locally, but the real cause may lie in how your foot and ankle manage force during movement. Learn how foot mechanics, tendon loading and gait influence heel pain, plantar fasciitis, posture and movement efficiency.
Most people think stress is all adrenaline and action.
But there’s another version — the quiet one. The one where motivation fades, energy drops, and your nervous system stops fighting and starts conserving.
This isn’t weakness. It’s biology.
Research from Martin Seligman and earlier work by Curt Richter showed that when stress becomes uncontrollable, the brain shifts into a shutdown pattern known as learned helplessness.
At a chemical level, this state is linked to altered acetylcholine signaling, increased nitric oxide, reduced thyroid hormone activity, and impaired mitochondrial energy production. In simple terms? Your metabolism and your mood are having the same conversation.
The good news: the nervous system is plastic. Environment, light exposure, movement, social connection, and metabolic support all influence whether the brain adapts toward resilience — or surrender.
Helplessness isn’t a character flaw.
It’s a reversible physiological state.
Tendon pain doesn’t heal with rest alone. Modern research shows tendons need the right kind of load, at the right time, to recover. This article breaks down what actually works — using the latest evidence from leading tendon researchers — and explains why rehab advice often sounds confusing but isn’t wrong.
I think people are expecting to be fixed in one session and people don’t realise the amount of joints and muscle connections in the lower body and the work needed (strength) and connectiveness (joint sequencing) to actually have a foot or lower limb function in walking.
The lower limb is not a single joint or muscle problem. It is a highly complex, multi-joint system that relies on precise timing, coordination, and load sharing between joints, muscles, tendons, ligaments, and the nervous system (Neumann, 2017; Standring, 2021).
Many people expect foot or knee pain to be “fixed” in one session.
But walking is a whole-body task involving nearly 78 joints, the nervous system, and connective tissue that adapts slowly over time. This article explains why real change takes longer — and why that’s exactly how lasting results happen.
Riccardo Galeotti doesn’t treat pain by chasing symptoms — he looks at how your body actually moves. As the founder of The Body Lab Canberra, Riccardo combines biomechanics, gait analysis, movement therapy, and acupuncture to uncover the patterns driving recurring pain. By focusing on how you walk, load, and adapt to gravity, his work helps clients move better, feel stronger, and build long-term resilience — not just short-term relief.
Most cholesterol is made inside your body, not eaten. This article breaks down how LDL and HDL actually work, why saturated fat isn’t the whole story, and why movement, muscle, and metabolic health matter far more than your choice of spread.
Struggling with foot pain in Canberra? Learn when arch support actually helps, when it doesn’t, and why foot function matters more than arch shape.
Back pain is ridiculously common in Canberra — but that doesn’t mean you should put up with it. In this guide, we break down the real causes of back pain, when you actually need a scan, who to see, and why movement (not bed rest) is your secret weapon. Clear, evidence-based, and written with zero fear-mongering — just the facts, a little sass, and practical steps to start feeling better today.
“Neutral spine” isn’t stiff posture — it’s your spine’s stress-free, pain-free position. This blog explains what it is, how to find yours, and why it changes everything from walking to lifting. With clear demos, simple cues, and a link to our Core Reset: Spinal Mobility Program, you’ll learn how to move better, breathe better, and feel better.
Can you really fix years of bad posture? Yes — absolutely. Your body is adaptable at any age, and with the right movement strategy, strengthening, mobility work and expert posture assessment, long-term improvements are not only possible but surprisingly achievable. Learn how to correct rounded shoulders, forward head posture, pelvic tilt and spine stiffness, and why clients across Canberra come to The Body Lab for posture and movement therapy.